Living with eczema and psoriasis: Children
- Living with eczema and psoriasis
- Living with eczema and psoriasis: Children
- Psoriasis and eczema for children - rules for moisturizing
- Adults - Care and anti-itching tips
- Living with eczema and psoriasis: Adult
- Psoriasis and adult eczema - rules for moisturizing
- Psoriasis and eczema in children: suitable hygiene
- Psoriasis and eczema in adults: suitable hygiene
- Children - Care and anti-itching tips
Living with eczema and psoriasis: Children
Eczema and psoriasis: the particular sensitivity of children Being affected by eczema or psoriasis is an almost permanent source of discomfort. Especially for the very young. Itching, lack of sleep, stress, sometimes teasing... these two diseases impact their quality of life. Together you can overcome this ordeal.
Updated on , validated by the medical directorate.
Psoriasis and eczema in children: what are the differences?
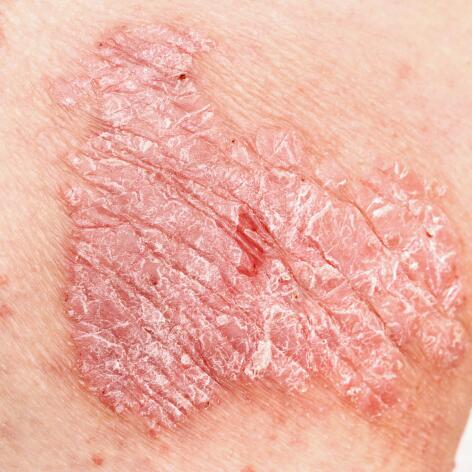
Psoriasis generally occurs in genetically predisposed individuals. It is manifested by an excessively rapid renewal of the epidermal cells and chronic inflammation of the skin.
Eczema, on the other hand, is a combination of an altered skin barrier and a greater sensitivity of the immune system to allergens, which makes the skin more reactive.
While they differ in their causes, the two conditions are similar in many ways. Both are chronic diseases marked by alternating flare-ups and periods of remission. The plaques are red and can be very itchy. While psoriasis in children is not very common, atopic eczema affects 10-15% of children under 7 in Europe.
Psoriasis and eczema in children: the signs that do not deceive
Flare-ups are marked by the appearance of plaques.
In psoriasis, these lesions are red and scaly. In children, they rarely itch and mainly affect areas where there is friction: elbows, the back of the forearms, knees, legs, lower back. They can also affect the scalp, eyebrows, ear canals. Or even the nails, the palms of the hands or the soles of the feet.
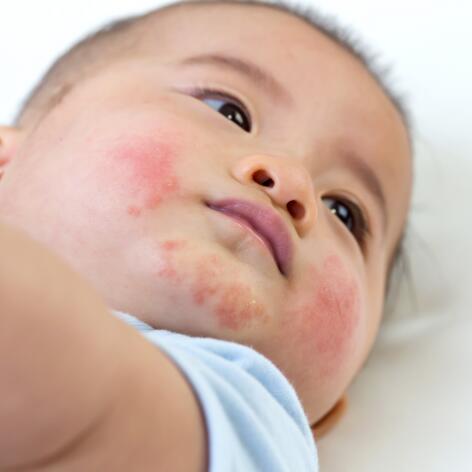
On the other hand, atopic eczema patches (which develop usually in infants and children) are often less thick, less well-defined and less scaly than psoriasis plaques. However, they are itchy. In children under one year of age, they affect certain parts of the face (forehead, chin, cheeks) and limbs (legs, arms). Between the ages of one and two, eczema is more prevalent on the head, neck and flexion folds. In children over two years of age, it is the folds (neck, under the ears, elbows, knees, buttocks), hands, wrists and ankles that are affected.
Areas of the eczema - face and neck
Anti-itching tips for children

The itching and burning caused by these diseases is a real suffering for children, and quickly becomes a source of stress with a significant impact on their daily life.

How to react as
parents?
If your child suffers from atopic dermatitis or psoriasis, you know how difficult it can sometimes be to manage. What could be more discouraging than seeing your child suffer and not knowing how to help? Above all, even if these diseases have a hereditary side, do not feel responsible. On the other hand, you have a role to play. You can support them and help them to cope. Talk to them, encourage them to express how they feel. It’s important not to minimise their discomfort. And of course, identify the triggers and take an active part in their care.
FRIENDLY (AND EXPERT) ADVICE
Pruritus, that unbearable itching sensation, is a vicious circle. In other words, the more your child scratches, the more they will want to scratch. But it’s very difficult to forbid a child not to touch their patches. Fortunately, there are alternatives. When it itches, encourage them to scratch their cuddly toy, take their mind off it by doing some physical activity...

What are
the treatments?
Treating eczema or psoriasis involves three key players: your child, yourself as a parent, and your doctor. First and foremost, only a medical examination (by a paediatrician, dermatologist or GP) will enable a clear diagnosis to be made, the disease to be better understood, and the most effective treatment to be put in place. This will depend on several factors, such as the impact on quality of life and the severity of the symptoms.
How can eczema and psoriasis be prevented?
In addition to treatment, you can take action to prevent flare-ups and itching. Prevention is based on three pillars that will help your child feel better. The first of these pillars is moisturizing. An emollient or moisturizing treatment will restore the skin's barrier function and prevent a new outbreak. You can find out all about it in our Spotlight on moisturizing rules.
Second pillar: proper hygiene. Many parents think that it’s better to space out the baths or showers of children affected by eczema or psoriasis. Yet hygiene is necessary. So how can we avoid irritating the skin when washing? Find the answer in our Spotlight on proper hygiene.
The last pillar: avoid scratching to avoid damaging the skin. Not an easy task. But don't worry. Here again, simple solutions exist, such as the use of smooth pebbles. See our dedicated spotlight.

ECZEMA AND PSORIASIS IN CHILDREN: OUR ANSWERS TO YOUR QUESTIONS
To sort the true from the false: that's what we're here for.
This is a very old belief... but it's just a belief. Neither condition is contagious. They are both chronic, inflammatory diseases. They are caused by skin abnormalities and environmental factors such as allergens...
Unfortunately not. The existing treatments and care are to deal with the symptoms. They are very effective, but their aim is not to make the disease disappear once and for all, but to treat the symptoms during the acute phase and to prevent the occurrence of new flare-ups.
Yes, it does. Stress affects the immune system. It can make a flare-up worse or trigger one.
Yes, of course. Be careful, however, as chlorine and salt can be irritating. Your child should therefore follow a few instructions. The first is to apply a barrier cream before swimming. It will protect the skin. Then rinse with fresh water after swimming. Lastly, apply an emollient care product before getting dressed.
Spa treatments are often recommended for atopic-prone children or those suffering from psoriasis. They include thermal spring water-based treatments (baths, showers, drinking cures, etc.), health education workshops which provide an opportunity for the child and their parents to learn more about the skin condition and its treatments, as well as regular medical follow-ups.
Our solutions for young, atopic skin
Eau Thermale Avène skin care products designed to help your child feel better in their skin
TO BE CONTINUED
- PsoriasisPsoriasis
Psoriasis is caused by an excessive and accelerated renewal of the outermost layer of the skin, combined with an inflammatory reaction. In its form and in the areas it affects, this disease has several aspects. Let's take a closer look at its causes, characteristics and treatments.
NEWSLETTER
Always here for your skin!
All our tips on how to take care of it every day.
Which skin care routine should you adopt?
Identify what it really needs with the help of our experts and discover the most suitable skin care routine for you.